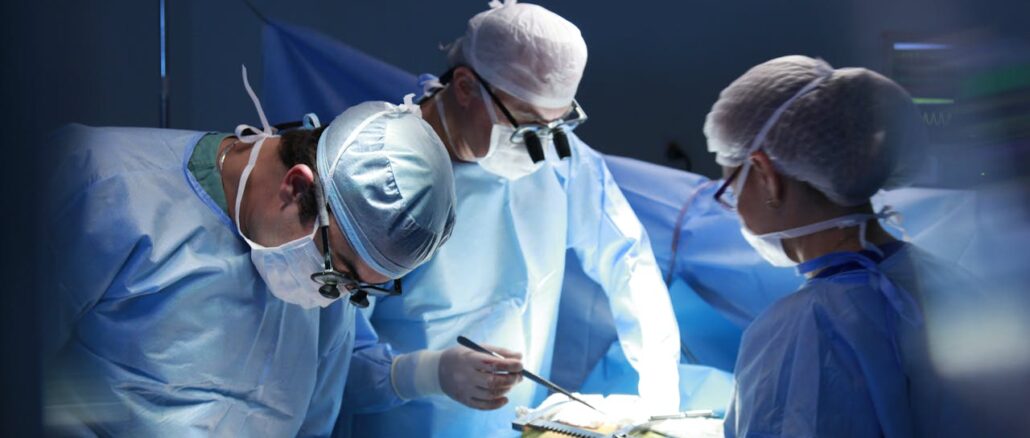
In surgery, people often judge performance by visible skill. They picture precision, speed, and technical mastery under pressure. Yet some of the most important work in an operating room happens through conversation. The steady exchange of observations, concerns, confirmations, and small warnings can shape a patient’s experience just as surely as any instrument on the table. That is one reason Dr. Barbara Robinson has long viewed communication between surgeons and nurses as one of healthcare’s most overlooked performance drivers.
This perspective does not treat communication as a pleasant extra or a matter of workplace chemistry. It treats it as part of the clinical process itself. When teams communicate well, they are not simply being polite. They are building a structure that supports safer decisions, smoother procedures, and more reliable care. In that environment, important details are less likely to be lost, concerns are more likely to be raised in time, and the operating room becomes a place where performance is shared rather than carried by a single person.
The Real Work Starts Before the First Incision
A surgical procedure may appear to begin when the first incision is made, but the real tone of the case is often set well before that point. It begins in the brief exchanges that happen before the patient is wheeled in. It begins when nurses and surgeons review the plan, raise questions, and make sure each person understands both the routine flow and the possible complications.
These moments rarely attract public attention, yet they can determine how well the rest of the day unfolds. A nurse may notice a detail in the patient’s history that deserves renewed attention. A surgeon may clarify a decision that helps the team prepare the right equipment in the right sequence. A simple question asked at the right moment can prevent confusion later, when time feels tighter, and the stakes feel higher.
This is where Robinson’s thinking stands out. Rather than focusing only on dramatic moments of crisis, the emphasis falls on the habits that prevent those crises from developing. Strong communication creates a kind of quiet readiness. It helps teams anticipate instead of merely react.
Why Nurses Often Hold the Missing Piece
One of the most undervalued truths in healthcare is that nurses often carry a broader view of the patient’s condition across time. Surgeons may lead the procedure, but nurses are frequently the ones who notice patterns, subtle changes, and practical concerns that do not always fit neatly into a chart. They see how a patient presents before surgery, how family concerns surface, how symptoms evolve, and how recovery begins to take shape.
When that perspective is welcomed, the team gains depth. When it is brushed aside, the team becomes narrower just when it should be at its strongest.
That dynamic matters because surgery is not only a technical event. It is also an information event. Every person in the room is working with data, whether that data comes from monitors, lab results, prior experience, or direct observation. A nurse who feels comfortable speaking up is not disrupting the process. That nurse is contributing to the full clinical picture.
The best surgical teams understand this instinctively. They do not treat communication as a hierarchy issue. They treat it as a patient safety issue.
Performance Is Built Through Trust
High-performing teams are rarely built on expertise alone. They are built on a trust strong enough to survive pressure. In an operating room, trust shows up in practical ways. It appears when a nurse flags a concern without hesitation. It appears when a surgeon listens without defensiveness. It appears when questions are answered clearly, and instructions are given in a way that leaves no room for guessing.
This kind of trust does not happen by accident. It is built through repeated behavior. Teams learn, case after case, whether speaking up is welcome or risky. They learn whether concerns are taken seriously or quietly ignored. Over time, those experiences shape the room’s culture.
That is why communication influences performance so deeply. A team that trusts one another can recover more quickly from the unexpected. They can adapt without panic. They can correct small problems before those problems grow larger. In contrast, a tense or dismissive environment slows everything down, even when no one says so out loud.
Hospitals often talk about efficiency in terms of scheduling, staffing, and equipment. Those factors matter. But efficiency is also affected by the emotional and professional climate in which people work. If communication is strained, delays grow more likely. If communication is clear, the work moves with greater steadiness.
The Hidden Link Between Communication and Burnout
There is another side to this conversation that deserves more attention. Strong communication not only affects patients. It also affects the people providing care.
In many clinical settings, burnout is discussed as though it comes only from long hours and high volume. Those pressures are real, but they are not the whole story. Burnout also grows in environments where professionals feel unheard, dismissed, or disconnected from their teams. A nurse who repeatedly notices something important but feels unable to say it carries a different kind of strain. A surgeon working in a tense room where communication is fragmented also feels the strain.
By contrast, a well-functioning team creates a sense of shared purpose. It reminds people that they are not carrying the burden alone. That matters more than many institutions realize. Respectful communication can reduce friction, improve morale, and make difficult work feel more sustainable.
This is one reason Barbara Robinson, MD, has drawn attention to communication as a performance issue rather than a personality issue. Framing it that way changes the conversation. It moves the topic out of the realm of vague workplace ideals and into measurable operational strength.
A Better Definition of Surgical Excellence
For years, healthcare culture has often celebrated the image of the singular brilliant surgeon. There is a reason that image persists. Skill matters, decisiveness matters, and leadership matters. But modern care is too complex to rest on one person’s talent alone.
A better definition of excellence includes how well a surgeon works with the team. It includes whether nurses are invited into the flow of decision-making. It includes whether briefings are clear, whether debriefs happen honestly, and whether the room makes space for useful dissent before a preventable mistake takes shape.
That broader definition may not sound glamorous, but it is closer to reality. Surgical excellence is not just about what one pair of hands can do. It is about how well a roomful of trained professionals can think together under pressure.
The Conversations That Change Outcomes
Some of the most powerful changes in healthcare do not arrive in the form of new machines or dramatic policy shifts. Sometimes they begin with a different kind of conversation. A more focused handoff. A clearer preoperative briefing. A nurse who is encouraged to trust her observation. A surgeon who understands that listening is part of leadership.
That is the heart of this perspective. Communication in the operating room is not background noise. It is part of the system that protects patients and supports the people caring for them. When hospitals treat it with the seriousness it deserves, they often discover that one of their strongest performance tools has been there all along, waiting to be used with greater intention.
Photo by CARLOSCRUZ ARTEGRAFIA:

